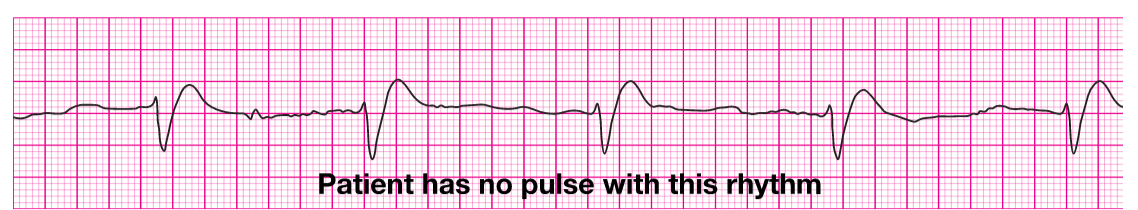
Look for: a history of thoracic trauma or invasive cancer, pulses not palpable during CPR, and jugular venous distention. Treat with: intubation, activated charcoal, antidotes specific to ingestion (naloxone for narcotics and sodium bicarbonate for tricyclic antidepressants), and hemodialysis for certain agents. 
Look for: a history of ingestion, empty bottles at the scene, abnormal neurologic exam, bradycardia, tachycardia, and a prolonged Q-T interval. Treat with: remove from the cold environment, perform active internal rewarming, and limit defibrillations to one attempt and withhold cardiac medications until the core body temperature is raised above 86☏ (30☌). Look for: a history of recent exposure to cold environment and low core body temperature. 
Hypothermia (spontaneous or environmental) Treat with: calcium chloride and sodium bicarbonate for hyperkalemia, and cautious infusion of potassium and magnesium for hypokalemia. Look for: a history of renal failure, recent dialysis, diuretic use, and abnormal ECG findings. Treat with: effective oxygenation and ventilation first, then consider sodium bicarbonate. 
Look for: a history of diabetes, such as hyperglycemic ketoacidosis, suggestive blood gas readings, bicarbonate-responsive preexisting acidosis, and renal failure. Treat with: effective oxygenation and ventilation. Look for: profound cyanosis, suggestive blood gas readings, and airway problems. Treat with: give a 500ml bolus of normal saline and then reassess. Look for: a history of trauma or severe dehydration, flat jugular veins, and ECG is rapid with narrow ORS complexes. In this Word section, we're going to take a closer look at the H's and T's, since they are so vitally important in treating PEA and other types of cardiac arrest. A Word About the Underlying Causes of Cardiac Arrest However, in order to correct PEA, the ultimate goal will always be to identify and treat the underlying cause of the cardiac arrest. The primary medication to treat PEA is 1mg of epinephrine 1:10,000 concentration every 3 to 5 minutes via rapid IV or IO push. Treatment involves high-quality CPR, proper airway management, IV or IO therapy, and the appropriate medication therapy. Pro Tip #2: Remember, pulseless electrical activity is not a shockable rhythm. In these two cases – hypovolemia and hypoxia – it's vital to recognize the condition early and treat for it quickly with volume replacement and oxygen therapy. Which is why it's important to look for evidence of these problems as you assess the patient. Of the H's and T's, hypovolemia and hypoxia are the two most common underlying and potentially reversible causes of PEA. The most common causes of cardiac arrest are presented as H's and T's as indicated below. As healthcare providers, you should memorize the list of common causes to keep from overlooking an obvious cause of PEA that might be reversed by appropriate treatment. In addition to CPR, identifying the underlying causes early, such as the H's and T's, and providing treatment quickly, is the key to reversing most pulseless electrical activity.Īs mentioned above, some of the more common reversible causes of PEA can be more easily remembered by the H's and T's. Remember, performing high-quality CPR is the initial treatment for PEA. So, it's really important to closely monitor the patient's pulse, blood pressure, and any underlying conditions he or she might have. Pro Tip #1: Any rhythm can deteriorate into PEA.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
